The healthcare management faced a tough situation during the pandemic time and emerged victorious in extending the best care to COVID & Non-COVD patients as well as safeguarding its medical care providers (clinical & non-clinical); and with the understanding that technology-driven practices and contact-less patient care are the new norms and necessity.
Today, medical technology integrated with deep learning and artificial intelligence is one of the major contributing factors. Online consultation through telemedicine, teleradiology, drone services, e-pharmacy, remote working, and at-home services are some of the examples contributing to reduced or no exposure. Radiology was among the forerunners that made a swift adaption to new norms and supported the system with remote working. The technology companies too supported the medical system’s functionality either in maintaining or increasing the efficiency of the operational team during the patient flow surge.
Teleradiology system driven by technological advancement has emerged as one of the most reliable modes of the patient care system in any given situation to deal with, be it a reporting for emergency or isolated COVID patients or IP/OPD patients, and could cope with the surge in image reporting through the option of remote reporting. This hybrid work norm supported many institutions in delivering patient care without any delay. Today’s teleradiology is integrated with the latest PACS, AI-enabled workflow, internet connectivity with wide bandwidth, and an experienced back-end support team that has made the reporting possible with short TAT. Technology companies have developed systems to transfer and archive large datasets with integrity fulfilling the radiologist’s need for high-quality images for reporting.
Machine Manufacturers are also contributing by developing systems that capture high-quality images with low-dose radiation and high sensitivity. To catch up with the trend of imaging services at point-of-care, compact mobile machines are being developed to fulfill the need. The ultrasound machine and mobile X-ray machines are proving it with their wireless and cloud-computing features.
Remote Learning is being embraced by educators and many clinicians. Online recorded or live sessions have become the mode of learning for aspiring future physicians and medical professionals. Webinars/conferences and interactive sessions are being conducted virtually benefiting healthcare providers and patients.
With progressing time, the positive and productive approaches of radiologists, healthcare providers, and technology companies the recovery from the pandemic is becoming a reality.
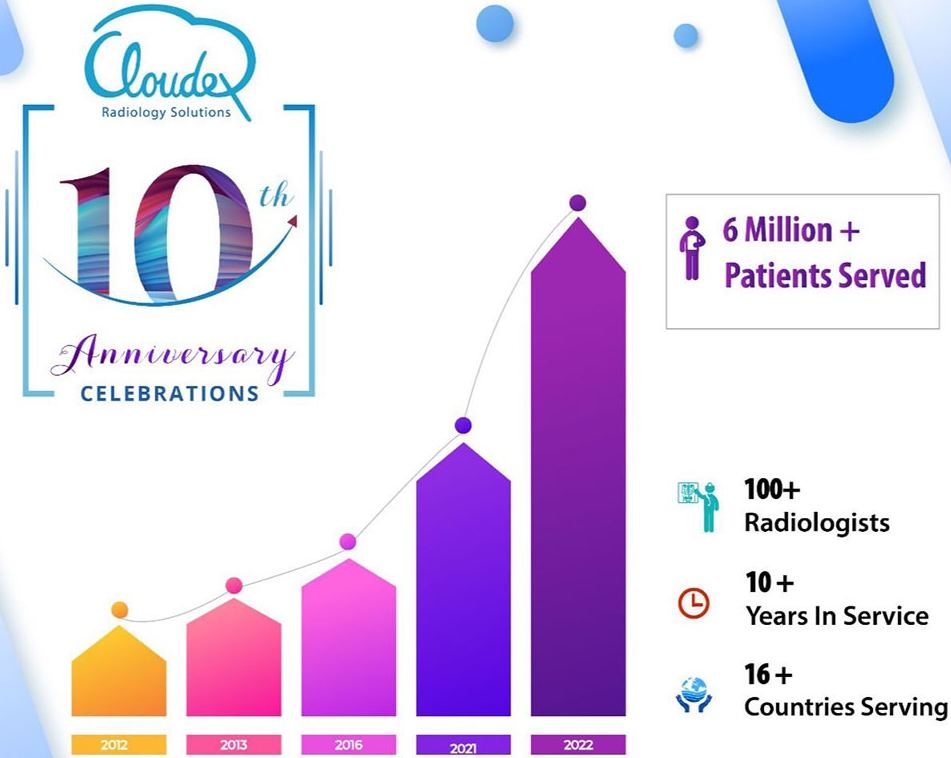
Cloudex Teleradiology Solutions during the Pandemic
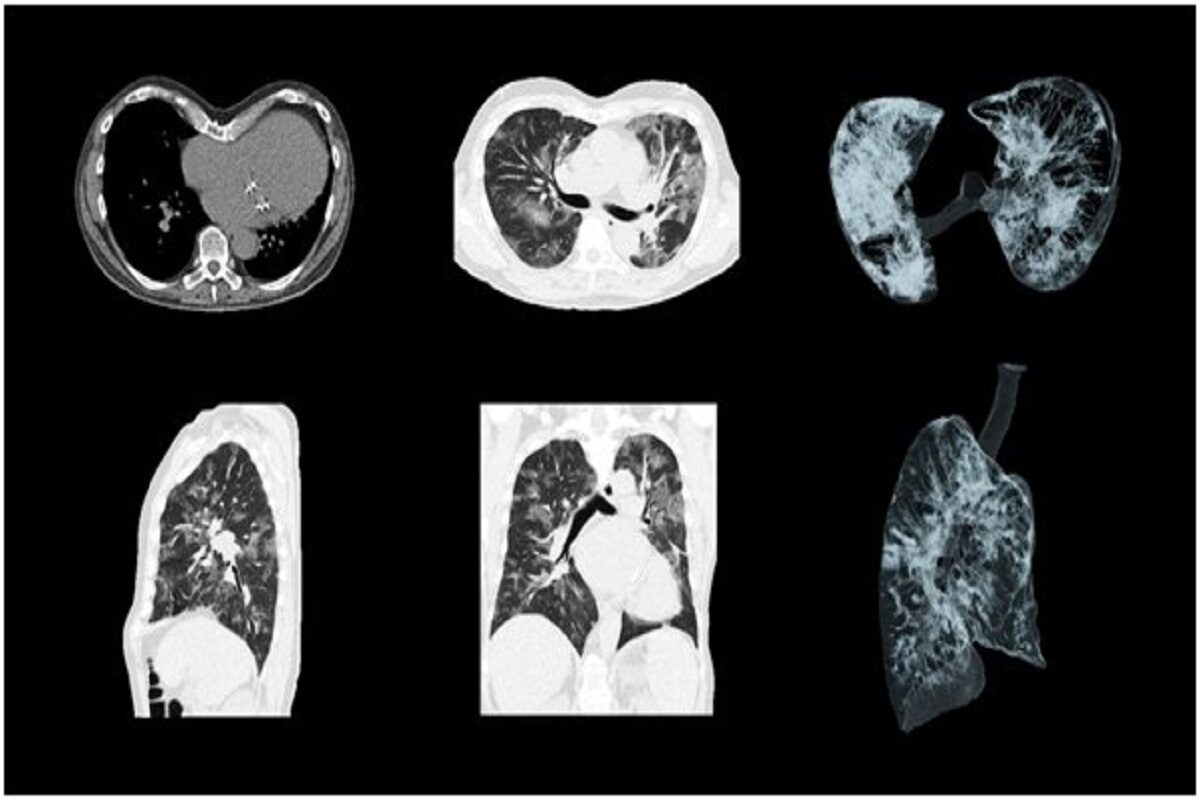
Cloudex with its advanced teleradiology service in India supported many health centers worldwide managing the patient surge with its prompt reporting services. The reporting was dominated by X-rays, CT, and MRI scans mainly for emergency cases as other patients were curtailed from outpatient services. Our experienced and expert teleradiologists team extended their much-needed services relentlessly around the clock. Safety measure guidelines were strictly followed by the back-end team while reporting was done remotely. The non-stop and timely service deliverance which includes subspeciality reporting in this crucial time helped many centers in facilitating patient recovery and saving lives and it turned out to be their winning edge.
At Cloudex, we support you to have that winning edge.