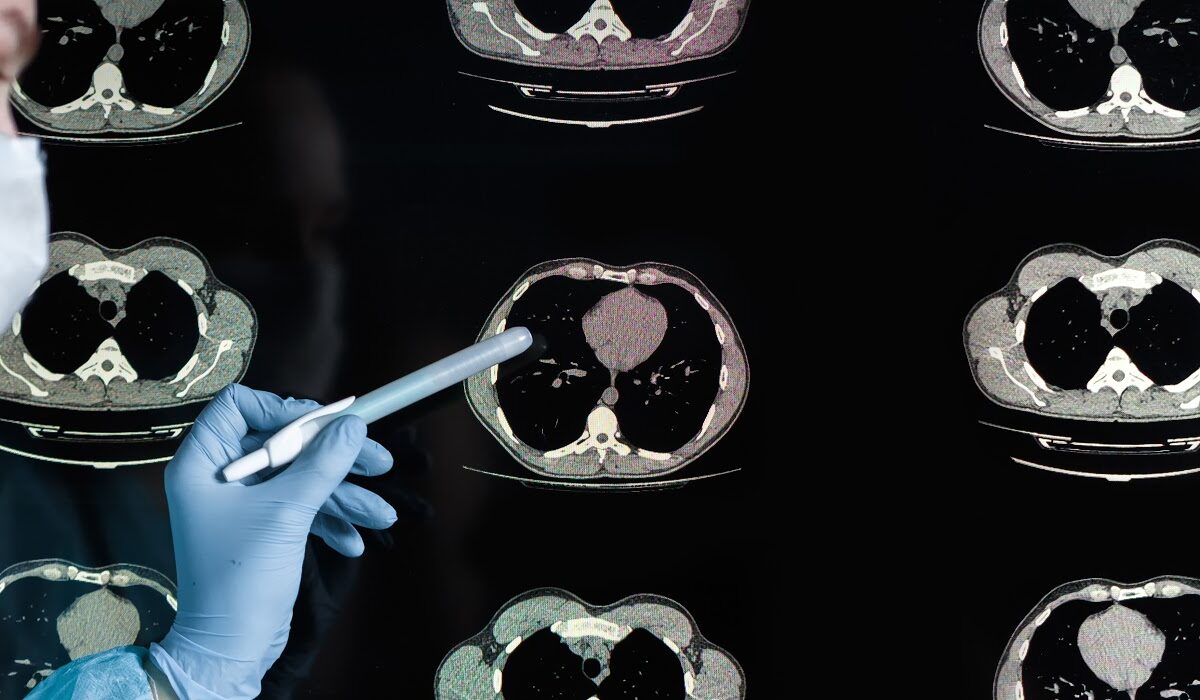
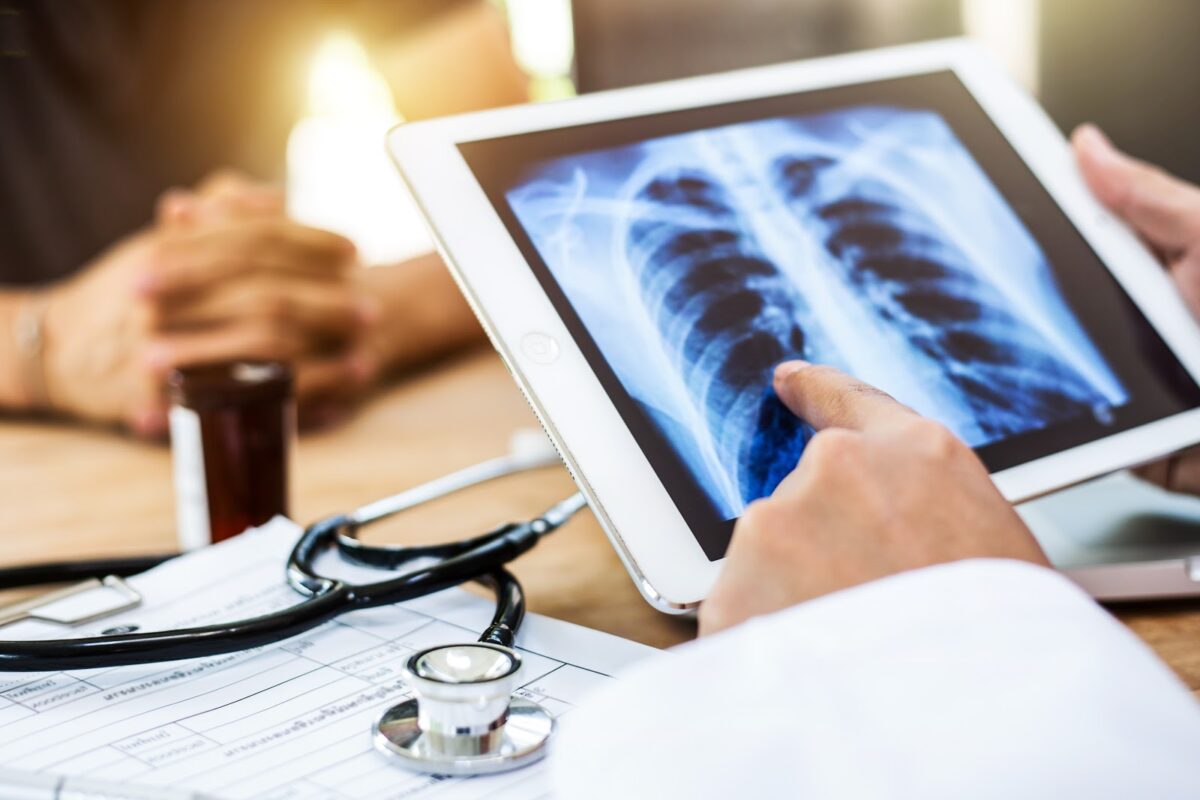
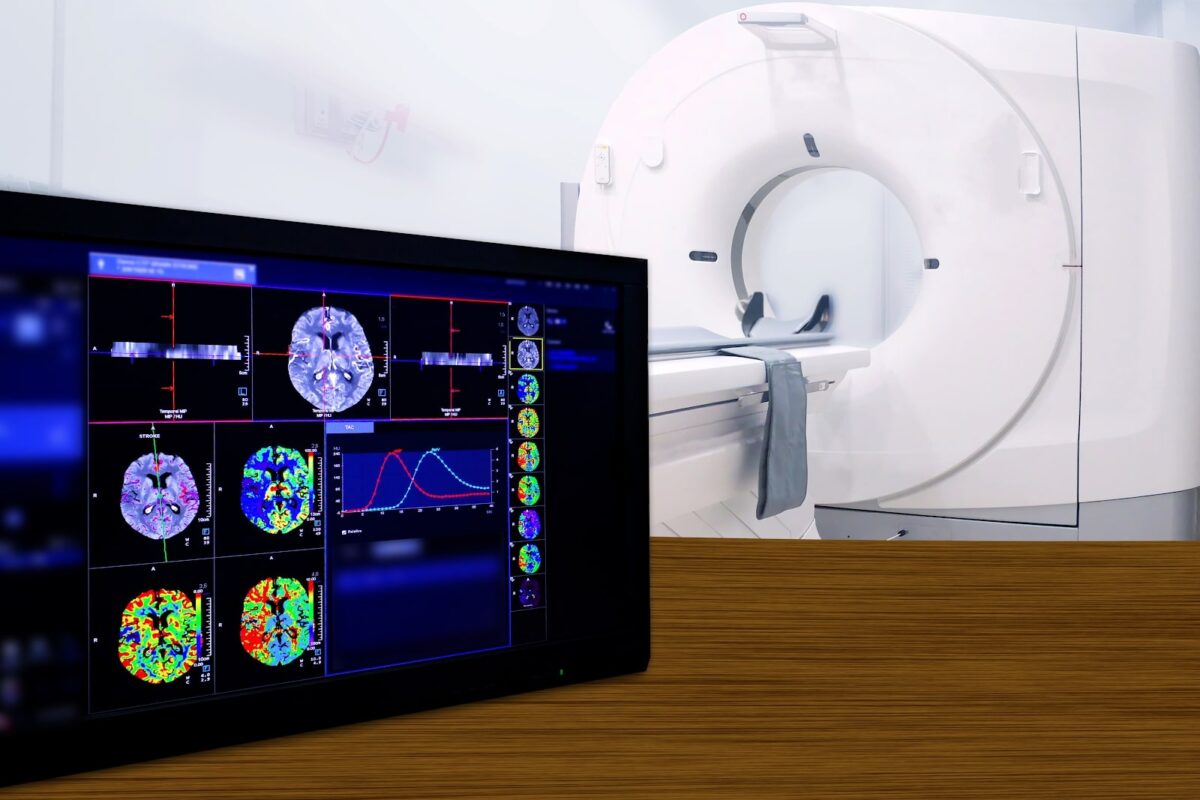
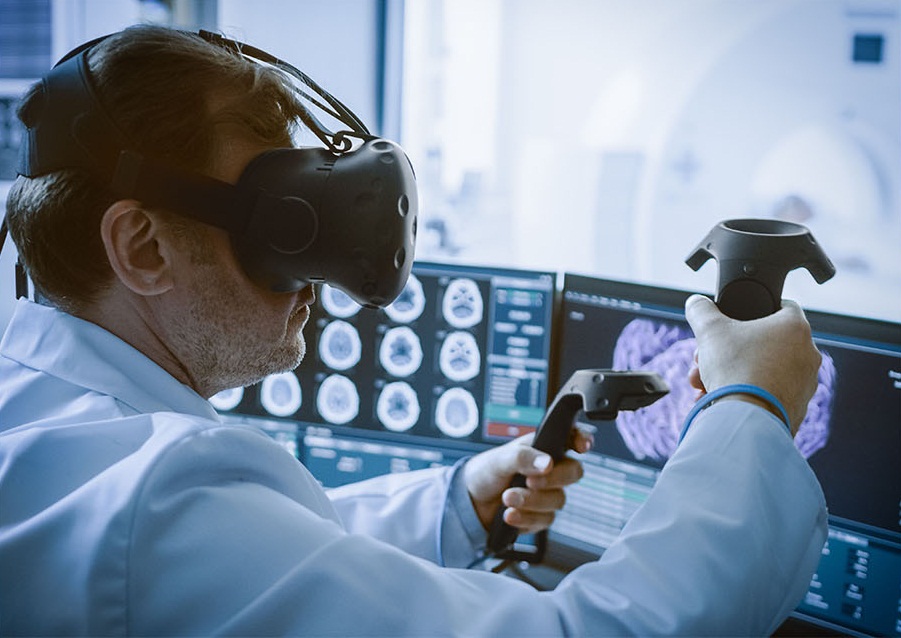
A medical system by which patient’s radiological images from a variety of health care facilities are transmitted electronically for review and reporting by experienced, offsite radiologists and that’s teleradiology. The resulting reports are then transmitted back to the original facility, providing key insights about the images and helping to determine the course of further patient care. The true fact is that this system is grown within the medical field over the last number of decades, only a few are familiar with the particulars of teleradiology.
Now in the present scenario use of teleradiology is highly recommended as the covid 19 crisis threatens the entire world. Moreover, it ensures the safety of professionals and patients simultaneously. However, optimization of IT solutions and implementation of the right change process is a significant milestone for a successful transition.
Radiology plays an important role during the pandemic as it is essential to maintain the continuity of the health service to the patients. Using such technology based on the transmission of radiological patient images from one location to another and allows radiologists to provide services without having to be in contact with the patient is peculiarly important to minimize the expansion of the covid 19 virus.
In some countries, radiology departments in public and private experienced this solution of remote working, showing a positive impact during the outbreak.
The physical distance between the technologist radiologist, the referring physicians, and the patient is of great advantage now as concerns the present situation. If the concerned patient is in self-quarantine due to exposure to a covid patient, in such situation teleradiology helps much with doctors as being able to read, albeit from far x-rays or CT scan of coronavirus patients.
In China at an early stage of a pandemic outbreak, before swab testing was really available, CT scan was used by doctors to assess the probability of covid 19 infections, same time used to track and monitor the progression of the disease as described by some researchers from China.
Teleradiology allows radiologists to work and be productive when isolated from the rest of their community, while the necessity for social distancing is inevitable in the current pandemic, definitely help to restrict the virus transmission. This practice of receiving images to interpret from a facility and that too is out of radiologists’ geographical vicinity is a truly valuable contribution at this time of unprecedented crisis. By supporting areas of the physician shortage and backing up they are in hospital counterparts, teleradiology serves in a significant way to relieve some of the stresses that global health care systems are currently experiencing.
Medical Science has proven time and again that when the resources are provided, great progress in the treatment, cure, and prevention of diseases can occur.
When there is a crisis we can use two brush strokes to write the word ‘crisis’. One brush stroke stands for danger and the other for opportunity. In a crisis, be aware of the danger but on the other hand recognize the opportunity. It’s really an unpredictable situation for the medical field globally, the danger is on the way we move on. But on the other side of the coin, we are forced to find innovative solutions to problems we may never face before.
When we approach the crisis from a hopeful perspective rather than with a stance of resistance, we can navigate this difficult situation by making it beneficial for the modern medical system knows to be teleradiology.